MMM Chiapas 2014: Successes and Lessons Learned

MMM 2014 Chiapas Team at the Hospital Básico Comunitario San Andrés Larráinzar (left to right): Bart White PA, Marty Kim MD, Rand Bourne, Ali Feinberg RN, Courtney Sherman RN, Sierra Bourne MD, Fru Bahiraei MD, Savannah Marks, Tim Crall MD, Kurt Smith MD, Kim Escudero MD, Karly Dawson PA, Scott McGuire EMT, Sara Morra PT, Brent Peterson NRP, Paul Chu MD, David Page, Gilann Bourne & Antonette Ciccarelli LVN. Photo by Sara B. May MD (behind the camera).
THE MAJORITY OF THE 2014 CHIAPAS TEAM arrived at LAX late Monday evening the 19th of May, after an intense and gratifying six days on the ground in San Andrés Larráinzar and San Cristóbal de las Casas. (We said goodbye to anesthesiologist Paul Chu and über-RN Ali Feinberg in Mexico City; Ali heading off to visit her parents in San Miguel de Allende, and Paul making his way back to Ohio via Miami.)
There were lessons learned, to be sure. They are noted below. But from an organizational standpoint, especially compared to past trips, this was a highly successful mission on a number of fronts:
1) TRANSPORT LOGISTICS:

Direct Relief International donated more than $18,000 worth of supplies and equipment to be used on this and future missions, including a $2,000 tabletop autoclave that was donated to the clinic in San Andrés.
Thanks to many weeks of hard volunteer work by Mike McMahon, Sara Morra, Jaymee Davis, Marty Kim and others, all medical supplies for this mission were inventoried, organized, and packed according to a fairly simple system that allowed us (Sara Morra, Loadmistress, in particular) to keep track of every last bag—59 total, including 20 flashy blue personal packs supplied by Black Diamond Equipment—from our HQ in Mammoth to LAX through customs in Mexico City all the way to the back room of a rural clinic in the highlands of Chiapas, and then back again. Though it was not perhaps essential on this trip, the separation of personal gear into recognizable and easily-carried backpack units made all transfers significantly tighter and easier than on past trips where we had all manner of personal duffels and roller bags mixed in with medical bags.
A single bag—a small duffel of toys and candies and such donated by our friends at the Mammoth Fun Shop—was briefly delayed by a pulled tag in Mexico City. Using our system we were quickly able to identify which bag it was, and to arrange its delivery to us in San Andrés the very next day. Remarkably, there were no misplaced passports and no chronic wanderings-off by members of the team.
LESSON LEARNED: Be sure to secure specific excess baggage allowance from airline at least a week before travel. We had such an allowance in place for the original November dates (postponed due to our deployment to the Philippines), and a vague promise for the same on this round, but in the end (both at LAX and on the return from TGZ) were forced to pay excess baggage fees on the order of US$5,000 to Aeromexico. Nb. As of 5/26 there is still hope that Aeromexico will step up and reimburse MMM for these charges.
2) LOCAL CONTACTS AND COMMUNICATION:
 We had in fact received from him, finally, one day before our departure from Mammoth, a series of official authorization letters from the Chiapas Secretary of Health and the regional Authority of Integral Family Development (DIF). Our longstanding misgivings were proven justified, however, upon arrival in Tuxtla-Gutierrez, when we learned that a crowd of 350 people had been assembled since early that morning at the DIF headquarters in San Cristóbal, waiting for the American doctors to begin triage (“valoraciones”). This despite the fact that we’d made and shared our airline reservations and clinic schedule numerous times over the previous three months—to arrive TGZ on Monday afternoon (1550hrs local time), to drive directly to San Andrés to set up camp and assess facilities that evening, and then to begin triage (in San Andres, NOT in San Cristobal) the following morning at 0800hrs.
We had in fact received from him, finally, one day before our departure from Mammoth, a series of official authorization letters from the Chiapas Secretary of Health and the regional Authority of Integral Family Development (DIF). Our longstanding misgivings were proven justified, however, upon arrival in Tuxtla-Gutierrez, when we learned that a crowd of 350 people had been assembled since early that morning at the DIF headquarters in San Cristóbal, waiting for the American doctors to begin triage (“valoraciones”). This despite the fact that we’d made and shared our airline reservations and clinic schedule numerous times over the previous three months—to arrive TGZ on Monday afternoon (1550hrs local time), to drive directly to San Andrés to set up camp and assess facilities that evening, and then to begin triage (in San Andres, NOT in San Cristobal) the following morning at 0800hrs.
 Our man had for some inscrutable reason failed to share this information with local authorities and had now spent the day lying to the crowd, explaining that we’d somehow been waylaid by customs in Mexico City.
Our man had for some inscrutable reason failed to share this information with local authorities and had now spent the day lying to the crowd, explaining that we’d somehow been waylaid by customs in Mexico City.
“There will be a revolt,” he announced to us upon arrival, “if you don’t commence surgeries tonight.”
Our Surgery Director, Dr. Fru Bahiraei, along with Medical Director Dr. Sara May and C.O.O. David Page were dispatched to San Cristobal in our man’s pickup truck to appease the throng (and to pay for two tanks of gasoline), while the rest of the team traveled the winding road up to San Andrés Larraínzar to establish camp per the original plan. The miscommunication(s) and their source were explained both to the assembled crowd and to the regional
LESSON LEARNED: We now have direct contact with and up-to-date information for the relevant players in the regional health establishment, including representatives from the Chiapas Secretary of Health, delegates from the regional DIF, as well as the Director and the Chief Administrator of the Hospital Básico Comunitario de San Andrés Larráinzar. We will now be able to work directly with these people, without an intermediary, which will undoubtedly make future missions much smoother in the planning and much more effective in their execution. Discussions are already underway for another medical/dental mission in one year (May 2015), with annual missions thereafter allowing for a greater educational component and exchange with local staff, and an ongoing improvement of systems and facilities. The goal being to work toward a greater range and sustainability of services in the Altos de Chiapas region even in our absence.
3) CAMP & ACCOMMODATIONS:
On previous missions to Chiapas, we’d relied on local authorities/officials to cover the cost of our accommodations in-country. This time, to avoid conflicts of interest, and the twice-daily, 45-minutes-each-way, car-sickness-plagued commute to and from San Cristobal, and because there are no lodging options to speak of in San Andrés—and also because we’ve made it a significant part of our organizational mission to train ourselves and our teams for the possibility of deployment in austere-environment/disaster scenarios—we’d resolved, on this mission, to set up our own self-contained camp adjacent to the clinic where we’d be working.
 Camping right on the clinic grounds spared us many hours of commuting. It gave us the flexibility to work late, for the surgeons to do after-hours rounds with patients and also to remain on call in case they were needed in the PACU. I believe it also sent a clear message to health officials, hospital staff and patients that the medical mission was our priority. And it gave us a chance, as time allowed, to settle into the rhythms of the village, to wander the streets in the fog and rain, to savor the brief vistas and the crowing of roosters at all hours of the night.
Camping right on the clinic grounds spared us many hours of commuting. It gave us the flexibility to work late, for the surgeons to do after-hours rounds with patients and also to remain on call in case they were needed in the PACU. I believe it also sent a clear message to health officials, hospital staff and patients that the medical mission was our priority. And it gave us a chance, as time allowed, to settle into the rhythms of the village, to wander the streets in the fog and rain, to savor the brief vistas and the crowing of roosters at all hours of the night.
LESSON LEARNED: Now that we’ve established a relationship with a local cook, we will be able to ensure on future trips that she has the appropriate facilities and enough of a deposit on the front end that she can do the majority of her shopping in San Cristobal before our arrival. This will allow her to prepare a much broader range of meals for the team. On future trips, the clinic director has promised to dedicate the entire (mostly unused) Casa Materna for our purposes, allowing us to establish and secure our own private kitchen, break and camp area.
4) O.R. SCHEDULING:

Triage Day: Dr. Tim Crall, orthopedic surgeon, maintains calm despite the press of patients. Dr. Kim Escudero, pediatrician, assists with discharge. Photo by David Page.
Triage is a difficult exercise even in the best of circumstances. A fine balance has to be struck between the unbridled ambition of surgeons (with their professed willingness to work 24 hours a day) and the constraints of circumstances and time—between on the one hand the desire to make a real difference/impact in as many patients’ lives as possible, and on the other the importance of avoiding procedures that might turn complex or risky. Neither do we want to leave patients needing serious followup that we will not be able to provide, nor do we want to end up turning people away for lack of time at the end of the week, after they’ve already been promised surgery.
In this case things were further complicated by the aforementioned flaws in pre-trip communication. Local administrators had not been given a clear sense of the scope of what we would be able to accomplish. And so the net had been cast wide. Radio advertisements had been broadcast throughout the greater region promising the possibility of everything from complete knee reconstructions to cosmetic varicose vein stripping. There were several hundred people assembled in the waiting room and outside the hospital at 0730hrs Tuesday morning as we set up to do evaluations. The patients were not, unfortunately, all representatives of the neediest segment of the local population, either medically or socioeconomically. But they had all spent the previous day sitting around DIF headquarters in San Cristóbal, waiting for us. Many had traveled four or five hours two days in a row for a chance at free surgery by American doctors. We felt obliged to work with the population before us.
LESSON LEARNED: Over the course of numerous administrative meetings, and with the express support of the director of the clinic and the regional Secretary of Health, we were able to make clear that on future missions it would be incumbent on the local delegates and authorities, as their end of the bargain, to screen patients much more rigorously so that those assembled on triage day would in fact be drawn only from the neediest segment of the population and as much as possible only from the immediate surrounding region.
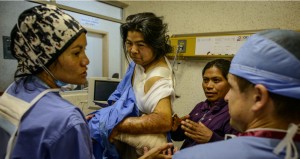
Dr. Kim Escudero translates for Dr. Tim Crall as he explains to a patient and her friend the use of a post-operative splint created by Dr. Crall and orthopedic PA Bart White to enhance the patient’s post-operative range of motion. Photo by Sara B. May
One by one, over the course of 8-9 hours, we saw and evaluated each patient (149 total, not counting the various groups of women with minor varicose or spider veins who were given group consultations and recommended compression stockings). They began at the intake desk, where ER physicians Sara May and Sierra Bourne wrote down individual names and complaints, gave each patient an intake form/SOAP note (designed by Sara May), and then directed him or her to one of three consultation rooms: OB/Gyn, Orthopedic Surgery (“Traumatología”) or General Surgery. The surgeons determined which cases they would safely be able to do with the tools and the time we had, and patients were either told immediately that there was nothing we could do, or asked to return at 1800hrs to see if their name was on the schedule for surgery in the coming days. By about 1830hrs we were taping to the wall a series of O.R. schedules for the next three and a half days totaling 57 surgeries.
LESSON LEARNED: The pressure to schedule more surgeries than can reasonably be accomplished within the time frame of a week-long mission, especially given the wide range of variables in a simple rural clinic, cannot be overestimated. Surgeons must not be allowed to promise surgery to any individual patients until all patients have been seen and evaluated, and until a final schedule has been devised in consultation with nursing/turnover, admin, and anesthesia teams. In this case, due to power-outage, a shortage of vents, and delays in instrument sterilization and room turnover, we were forced, on Surgery Day 2, to cancel four gall bladder cases. Luckily we were able to do this with some anticipation rather than at the very end of the mission with those patients already having waited all week. And still, the general surgery team worked until 0300hrs that morning, only to start back up again five hours later.
5) PATIENT CONTROL AND RECORD-KEEPING:
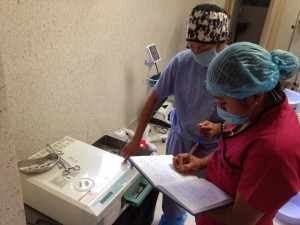
Dr. Kim Escudero and head nurse Marisela de Jesus Bautista run through the paces on the clinic’s new autoclave, donated by Direct Relief.
Once a patient’s name and procedure was on the surgery schedule, with his or her intake form (SOAP note) filed in the appropriate three-ring binder according to specialty (again: OB/GYN, ORTHO or GEN), a separate “Intra-Operative Form” was started. This form was used by our anesthesiologists Paul Chu and Kurt Smith for their pre-operative patient interviews, then passed to the appropriate O.R. circulator for note-taking during surgery. Post-operative notes and instructions were made on a separate sheet by the surgeon to be translated by our PACU nurse for local recovery nursing staff. Our dedicated Scribe, Savannah Marks, kept track of all this documentation and was able to deliver final reports even before we left Chiapas.
LESSON LEARNED: Communication of post-operative instructions and coordination with successive shifts of local recovery nursing staff was dramatically improved once Antonette Ciccarelli, with her excellent handle on medical Spanish, took charge of this. On future trips we need always to have at least one RN (with translator if necessary, and pre-printed Spanish-language instructions) dedicated to the PACU/recovery/discharge end of surgeries.
6) SUPPLIES, STERILIZATION AND TURNOVER:
This was without a doubt the primary source of bottlenecks in our surgery schedule. Our two anesthesiologists were able to keep up, even with three tables in use at a time and only one functioning vent. A brand new tabletop autoclave donated to us by Direct Relief International proved invaluable for flash-sterilizing key surgical instruments. And yet there were times when instruments were lost track of, or mixed in with other sets. Not infrequently the main autoclave staff would send an instrument back for more scrubbing before sterilization. And many times we ended up waiting for something essential to emerge from the 2-hour cycle in the main autoclave (which machine was great when it was working, but then not so great when it didn’t work for hours one morning while the hospital was switched over to generator power).
LESSON LEARNED: We need to have one or two personnel, each with a good working knowledge of O.R. supplies and instruments, dedicated at all times to overseeing cleaning staff, working with the autoclaves/staff and generally keeping track of instruments and supplies from the end of one procedure to the beginning of the next. It’s not necessarily the most glamorous position. But it is among the most important.
7) PATIENT NUMBERS:
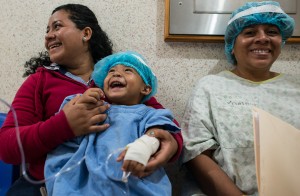
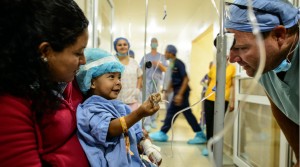
“It’s always gratifying to know that we are helping the most innocent of the populace who have no voice or control over their lot in life,” writes anesthesiologist Kurt Smith. “Children are often the most benefitted from these missions.” Photo by Sara B. May.
In three and a half days, the team was able to perform a total of 54 successful surgeries, representing all but four of the 57 surgeries scheduled after initial triage (four gall bladder surgeries were canceled on Day 2 for lack of time, and one ortho surgery was canceled due to patient no-show) plus a highly impactful skin release procedure performed by Dr. Fru Bahiraei and an added tubal ligation performed by Dr. Marty Kim. 109 patients were seen in general clinic by our ER Physicians Sara May and Sierra Bourne.
“One should always note the incredible acuity of many of the cases,” writes anesthesiologist Kurt Smith. “Most of them were much worse than anything we would ever see in the States because no patient would be made to wait so long until their medical problems were so far advanced. These types of cases only make the work much more difficult and hence time consuming.”
MMM Chiapas Patient Overview 2014 (pdf)
MMM Chiapas Surgeries 2014 (pdf)

MMM Chiapas 2014 Team with local hospital staff.






